Health
Colorado dropped people from Medicaid at a rate comparable to red states, alarming advocates for the poor
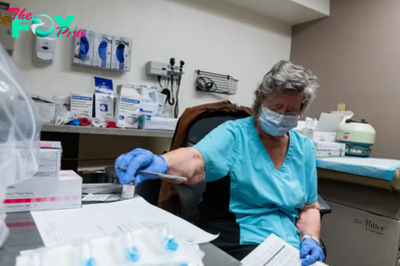
Colorado stands out among the 10 states that have disenrolled the highest share of Medicaid beneficiaries since the U.S. government lifted a pandemic-era restriction on removing people from the health insurance program.
It’s the only blue state in a cluster of red states with high disenrollment rates — a group that includes Idaho, Montana, Texas, and Utah — in the Medicaid “unwinding” underway since spring 2023.
Colorado also is the only state that had all the policy ingredients in place to cushion the fallout from the unwinding, according to Medicaid policy analysts at KFF.
But it seems the cushion hasn’t been deployed.
“There’s really a divide in Colorado between our progressive policies and our underfunded and fragmented administration,” said Bethany Pray, chief legal and policy officer at the Colorado Center on Law and Policy, a Denver-based legal aid group.
According to KFF data, during the unwinding Colorado has seen a bigger net drop in enrollment in Medicaid and the Children’s Health Insurance Program than any state except Utah.
Advocates for health care access, researchers, and county administrators — the administrators handling the bulk of the Medicaid redeterminations in Colorado — say that the major issues involve outdated technology and low rates of automatic renewals. Both create obstacles to enrollment that undercut the state’s progressive policies.
State officials have a rosier view. They say the drop in enrollment is a sign that they did a good job enrolling people at the height of the COVID-19 pandemic. Secondly, they say Colorado’s economy is doing well, so more people can get insurance through their jobs.
☀️ READ MORE
Colorado Medicaid problems still rampant as state agency tries to address computer, structure issues
Colorado Medicaid is discriminating against people with disabilities, federal complaint claims
Percentage of people without health insurance coverage in Colorado hits an all-time low
“When we have a really stellar unemployment rate, not as many people need safety-net programs, and we’re proud of that. Our people are rising and thriving,” said Kim Bimestefer, who leads the Department of Health Care Policy and Financing and is the state’s top Medicaid official. Her department has also said that some people choose not to fill out their eligibility paperwork because they know their incomes are too high to qualify.
Bureau of Labor Statistics data shows that while it’s true Colorado’s unemployment rate is lower than the nation’s as a whole, it’s higher than it was before the pandemic.
State officials say they believe Medicaid enrollments dropped because many of those people found jobs, as reflected by the lower unemployment rates. But that scenario happened in fewer than half of the state’s counties, a KFF Health News analysis found. Notably, in 11 counties where unemployment stagnated or increased from January 2020 to April 2024, the share of the population covered by Medicaid shrank. A low unemployment rate does not necessarily mean there is less of a need for Medicaid coverage, because many employed people earn wages low enough to still qualify for the program.
Colorado increased enrollment in Medicaid and the related Children’s Health Insurance Program by 35% during the covid public Health emergency, compared with about 30% nationally and among Medicaid expansion states.
“We grew more, which means, logically, we’re going to disenroll more,” said Bimestefer.“We went up higher, we’re going to come down lower, because our economy is stellar.”
Her department’s website initially claimed Colorado’s Medicaid enrollment grew more than any other Medicaid expansion state except Hawaii. But data from the Centers for Medicare & Medicaid Services shows pandemic enrollment growth in other states, including Indiana, North Dakota, Virginia, and Nevada, also exceeded that of Colorado.
Even if it had grown the most, the argument that what comes up must come down doesn’t hold water, Medicaid policy analysts said.
“A counterargument to that is we know that there was never a full participation in Medicaid prior to the pandemic,” said Jennifer Tolbert, deputy director of the KFF Program on Medicaid and the Uninsured.
Tolbert said she was surprised by the extent of Colorado’s Medicaid enrollment losses, given it was the one state in the nation that met all the criteria that KFF expected would cushion the effects of the unwinding. Those policies include adopting the Affordable Care Act’s Medicaid expansion and the automatic processing of renewals.
Tolbert was among several policy researchers who said that even if unemployment returned to pre-pandemic levels, they would expect a higher, not lower, share of Coloradans to be enrolled in safety-net coverage.
Ally Sullivan, a spokesperson for Gov. Jared Polis, a Democrat, said one complicating factor in Colorado’s system is that it’s among the handful of states where most of the eligibility verification work falls on counties, “which added complexity to the state’s unwind process.”
-

 Health6h ago
Health6h agoThe Surprising Benefits of Talking Out Loud to Yourself
-

 Health8h ago
Health8h agoDoctor’s bills often come with sticker shock for patients − but health insurance could be reinvented to provide costs upfront
-

 Health23h ago
Health23h agoWhat an HPV Diagnosis Really Means
-

 Health1d ago
Health1d agoThere’s an E. Coli Outbreak in Organic Carrots
-

 Health2d ago
Health2d agoCOVID-19’s Surprising Effect on Cancer
-

 Health3d ago
Health3d agoWhat to Know About How Lupus Affects Weight
-

 Health5d ago
Health5d agoPeople Aren’t Sure About Having Kids. She Helps Them Decide
-

 Health5d ago
Health5d agoFYI: People Don’t Like When You Abbreviate Texts