Health
Colorado doctors take on dental duties to reach low-income and uninsured patients
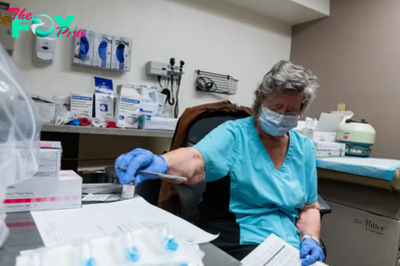
Pediatrician Patricia Braun and her team saw roughly 100 children at a community health clinic on a recent Monday. They gave flu shots and treatments for illnesses like ear infections. But Braun also did something most primary care doctors don’t. She peered inside mouths searching for cavities or she brushed fluoride varnish on their teeth.
“We’re seeing more oral disease than the general population. There is a bigger need,” Braun said of the patients she treats at Bernard F. Gipson Eastside Family Health Center, which is part of Denver Health, the largest safety-net hospital in Colorado, serving low-income, uninsured, and underinsured residents.
Braun is part of a trend across the United States to integrate oral health into medical checkups for children, pregnant women, and others who cannot afford or do not have easy access to dentists. With federal and private funding, these programs have expanded in the past 10 years, but they face socioeconomic barriers, workforce shortages, and the challenge of dealing with the needs of new immigrants.
☀️ READ MORE
What’s Working: Denver-based Guild’s CEO talks about AI, frontline workers and her new job
Controversial effort to impose stricter rules on Colorado charter schools fails in first vote
University of Colorado regents consider gun ban as concerns over campus safety mount
With a five-year, $6 million federal grant, Braun and her colleagues have helped train 250 primary care providers in oral health in Colorado, Montana, Wyoming, and Arizona. Similar projects are wrapping up in Illinois, Michigan, Virginia, and New York, funded by the federal Health Resources and Services Administration’s Maternal and Child Health Bureau. Beyond assessment, education, and preventive care, primary care providers refer patients to on- or off-site dentists, or work with embedded dental hygienists as part of their practice.
“Federally qualified health centers have a long history of co-locating dental services within their systems,” Braun said. “We’re taking that next step where care is not just co-located, meaning, say, we’re upstairs and dental is downstairs, but we’re integrated so that it becomes part of the same visit for the patient.”
Having doctors, nurses, and physician assistants who assess oral health, make referrals, and apply fluoride at community health centers is critical for the many children who lack access to dental care, said Tara Callaghan, director of operations for the Montana Primary Care Association, which represents 14 federally qualified health centers and five Urban Indian organizations.
“Providing these services during medical visits increases the frequency of fluoride application,” Callaghan said, and “improves parents’ knowledge of caring for their child’s teeth.” But obstacles remain.
Because of Montana’s large geographic area and small population, recruiting dental professionals is difficult, Callaghan said. Fifty of the state’s 56 counties are designated dental shortage areas and some counties don’t have a single dentist who takes Medicaid, she added. Montana ranks near the bottom for residents having access to fluoridated water, which can prevent cavities and strengthen teeth.
Pediatric dental specialists, in particular, are scarce in rural areas, with families sometimes driving hours to neighboring counties for care, she said.
Embedding dental hygienists with medical doctors is one way to reach patients in a single medical visit.
Valerie Cuzella, a registered dental hygienist, works closely with Braun and others at Denver Health, which serves nearly half of the city’s children and has embedded hygienists in five of its clinics that see children.
State regulations vary on which services hygienists can provide without supervision from a dentist. In Colorado, Cuzella can, among other things, independently perform X-rays and apply silver diamine fluoride, a tool to harden teeth and slow decay. She does all this in a cozy corner office.
Braun and Cuzella work so closely that they often finish each other’s sentences. Throughout the day they text each other, taking advantage of brief lulls when Cuzella can pop into an exam room to check for gum disease or demonstrate good brushing habits. Braun herself takes similar opportunities to assess oral health during her exams, and both focus on educating parents.
Medical and dental care have traditionally been siloed. “Schools are getting better at interprofessional collaboration and education, but by and large we train separately, we practice separately,” said Katy Battani, a registered dental hygienist and assistant professor at Georgetown University.
Battani is trying to bridge the divide by helping community Health centers in nine states — including California, Texas, and Maryland — integrate dental care into prenatal visits for pregnant women. Pregnancy creates opportunities to improve oral Health because some women gain dental coverage with Medicaid and see providers at least once a month, Battani said.
In Denver, housing instability, language barriers, lack of transportation, and the “astronomical cost” of dentistry without insurance make dental care inaccessible for many children, the migrant community, and seniors, said Sung Cho, a dentist who oversees the dental program at STRIDE Community Health Center, serving the Denver metro area.

STRIDE tries to overcome these barriers by offering interpretation services and a sliding pay scale for those without insurance. That includes people like Celinda Ochoa, 35, of Wheat Ridge, who waited at STRIDE Community Health Center while her 15-year-old son, Alexander, had his teeth cleaned. He was flagged for dental care during a past medical checkup and now he and his three siblings regularly see a dentist and hygienist at STRIDE.
One of Ochoa’s children has Medicaid dental coverage, but her three others are uninsured, and they couldn’t otherwise afford dental care, said Ochoa. STRIDE offers an exam, X-rays, and cleaning for $60 for the uninsured.
In the past year, Cho has seen an iNFLux of migrants and refugees who have never seen a dentist before and need extensive care. Medical exams for refugees at STRIDE increased to 1,700 in 2023 from 1,300 in 2022, said Ryn Moravec, STRIDE’s director of development. She estimates the program has seen 800 to 1,000 new immigrants in 2024.
-

 Health1d ago
Health1d agoTeens Are Stuck on Their Screens. Here’s How to Protect Them
-

 Health1d ago
Health1d agoHow Pulmonary Rehab Can Help Improve Asthma Symptoms
-

 Health1d ago
Health1d ago10 Things to Say When Someone Asks Why You’re Still Single
-

 Health2d ago
Health2d agoThe Surprising Benefits of Talking Out Loud to Yourself
-

 Health2d ago
Health2d agoDoctor’s bills often come with sticker shock for patients − but health insurance could be reinvented to provide costs upfront
-

 Health3d ago
Health3d agoWhat an HPV Diagnosis Really Means
-

 Health3d ago
Health3d agoThere’s an E. Coli Outbreak in Organic Carrots
-

 Health4d ago
Health4d agoCOVID-19’s Surprising Effect on Cancer